

Loma Linda, Cal. woman - one of the longest living heart transplant patients -undergoes a procedure to repair a rapid, irregular heartbeat. By Gigi Hanna - Sun Staff Writer
Marjorie Rorabaugh's electrical system had a short.
So last week doctors did the equivalent of soldering her transplanted heart.
The Loma Linda resident was getting dizzy and knew there was something wrong. As one of the longest living heart transplant patients -- she's had it almost 17 years -Rorabaugh is sensitive to any irregularitie s.
"I know my heart so well anymore that I know when I have a problem," she said. "I rarely have problems. Usually I dance in here (clinic), get checked and go on my way."
She didn't feel like dancing, though. She was even having problems standing up.
What doctors found was a rapid, irregular heartbeat that probably would have developed in the donor, had he lived long enough for it to develop.
 "He probably would have developed it eventually, but there's no way to predict," said Dr. Marc Platt, the electrophysiologist who operated on Rorabaugh.
"He probably would have developed it eventually, but there's no way to predict," said Dr. Marc Platt, the electrophysiologist who operated on Rorabaugh.
"It's something people are born with, that can develop over time for no reason other than the aging of the electrical system of the heart."
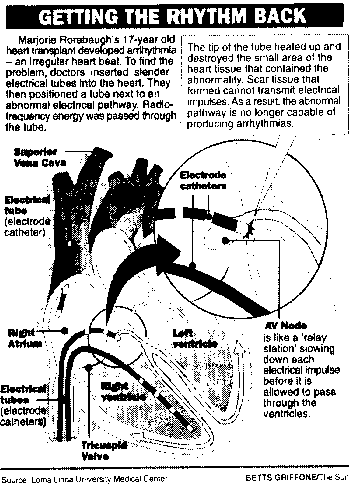
Few transplanted hearts develop it, Platt said. Rorabaugh took the news in stride: "Since I' ve taken over this heart, I' ve taken over his problem; but I'm glad to have it anyway." Platt performed an ablation, a non-surgical procedure that snakes catheters up from the groin and down from the neck to map the electrical activity of the heart and find the "short" in her system. Once it was located, Platt burned a pinhead-sized hole in the heart with radio frequency energy similar to microwaves to stop the arrhythmia.
During that, Rorabaugh went into cardiac arrest caused by clogged arteries, which is also rare, Platt said.
A stent, acting so mewhat like the children's toy "Chinese Handcuffs," was inserted into Rorabaugh's left coronary artery to prop open the collapsed vein.
Rorabaugh was a little leery of the procedure, but decided it was unavoidable. "I don't like the idea, but I have things to do and places to go," she said.
The eight-year Loma Linda resident is a volunteer at Jerry L. Pettis memorial Veterans Hospital where her husband is a patient in the nursing home.
Her health problems are a puzzle t o medical officials, who aren't used to seeing these kinds of problems in heart transplants.
"The whole thing is unusual because this is a transplanted heart," Platt said. "When you take a heart from a 20-year-old and put it into an older person, you're theoretically less likely to develop hardening of the arteries or other irregularities
"So that shows there' s some interaction between the heart itself and the new recipient," Platt said.
But just because her condi tions aren't often seen, doesn't necessarily mean they are rare, he said.
"There are not that many people who' ve had transplanted hearts that many years," Platt said. "This (condition) may develop naturally, but we just haven't been doing it all that long."
The San Bernardino County Sun 7/31/96
Contributed by Tx Stewart Lilley, Victorville, CA
 Editor's Note:
One of the wonderful things about heart and lung transplantation is that you meet such great fellow patients. When I was very new to being a Tx, Margie was already an old hand, but she was always sincerely interested in everyone at the clinics well-being and more than a few times offered advice that some side effects were more imagined than serious.
Editor's Note:
One of the wonderful things about heart and lung transplantation is that you meet such great fellow patients. When I was very new to being a Tx, Margie was already an old hand, but she was always sincerely interested in everyone at the clinics well-being and more than a few times offered advice that some side effects were more imagined than serious.
As longer UpBeat readers will remember, Margie had the first coronary artery bypass on a transplanted heart at the University of Arizona Medic al Center in 1988.
Now the above article doesn't make it very clear at all, but while Margie's arrhythmia was indeed serious, perhaps the most significant thing that came out of the surgery and investigation was the fact that except for one very localized area of blockage or stenosis in the coronary bypass, Margie's transplanted heart is in amazingly clear condition. They inserted a stint in the artery, which is again believed to be the first, and Margie is again ready for the road.
A former nur se, when asked she will willing state that she has led just as normal a life as possible since transplant. She has watched her diet, but really done nothing extraordinary, except being constantly active.
by Don Marshall
There is now a statistically significant group of heart and heart/lung transplants, who received their organs in the 80's, and have now successfully negotiated the potential pitfalls of transplantation for nigh on some 7 to 12 or more years. The purpose of the above statement is not to set up and"old boy, new boy" adversarial position, but rather to point out a medical fact that has perhaps not been brought home to those of us who may have mellowed just a bit with our attitudes toward the peculiarities of transplant care.
It is quite safe to say that all of us in this transplantation tenure group received the same initial 3 drug therapy -- cyclosporine (we were the original "plunger thumbs"), imuran and prednisone. And as we entered the 90's, the medical therapy protocol very gradually changed and prednisone no longer became the drug of choice it once was. A great effort was made to reduce or eliminate entirely the intake of prednisone by stable transplant recipients.
This was not a medically legislated change, but as is normal in all these instances was adopted center by center, and even then by degrees. Some centers were very strong on total wit hdrawal, others merely tried to reduce the prednisone to some "accepted" minimum.
Unfortunately, for some patients the time of this reversal of previously accepted treatment doctrine was too late. One group of these patients simply could not drop the use of prednisone, because as soon as the level dropped to a certain point, different for each individual, they would quickly go into allograft rejection.
Then there was another group whose bodies had become so totally adapted to the daily or regular intake of prednisone that their adrenal cortex effectively shut down on a permanent basis. When the prednisone was significantly reduced from the medication program of these patients their muscles became "weak" and their joints ached, and they seemed tired a great part of the time. This group had innocently developed, in this situation, an induced condition called chronic Addison's disease.
Now this is not one of those throw up your hands and whimper, "Oh no not again" situations. After all President Kennedy had Addison's disease and functioned rather well. However, because patients with Addison's disease cannot increase their output of corticosteroid hormones in response to stress, they are at risk during stressful situations such as infection, surgery, or injury. Their physicians must instruct them in the need for increased doses of corticosteroid drugs at such times, so that the body mechanisms that fight infection and promote healing are not impaired. (1)
Thus i n the event of a situation causing you to come under the care of a non-transplant team physician, it is essential for you to inform the doctor of your prednisone dependency. Failure to do so could result in serious damage to your body before the situation is rectified.
Obviously, in the worst case scenario one of us with the Addison's syndrome is taken to an emergency room either very ill or injured and in a semi-conscious condition. Hopefully the critical care physician will maintain a high index of suspicion for endocrine disease in all trauma victims. Realistically, it may be hours or even a day before your endocrine condition comes under review. The best solution would seem to be to carry a Med-Alert type card or MEDIC vial that contains all the information about your medications and chronic conditions. But most importantly, make sure your personal support family is aware of your need for additional corticosteroids in an instance of body stress. Even if a member of this group is not present with you in the hospital, they can call and advise of the requirement just as soon as they are notified of your situation. Very similar to organ donation, carry the information, but then make sure your loved ones and other supporting parties also know of your needs.
(1) The American Medical Association Home Medical Encyclopedia, ISBN 0-39458248-9 p.67
(2) Management Of The Trauma Victim With Pre-Existing Disease. Boulanger, BR; Gann DS Crit. Care Clin 1994 Jul; 10(3):537-54
A Surgical Alternative for Heart Failure and Transplantation Patients As seen on ABC's 20/20 Friday, June 14, 1996
Each year, 400,000 Americans are diagnosed with congestive heart failure, a condition in which the heart is not pumping as efficiently as it should. People with congestive heart failure become short of breath and tired if they exert themselves. If left untreated, congestive heart failure can result in damage to the heart muscle. Treatment varies with the severity of the disease, ranging from medications to heart transplantation. Currently, congestive heart failure is the third-leading cause of hospitalization in the country. Ventricular remodeling involves removing a portion of the enlarged heart muscle to relieve stress on the heart and improve its pump function. Patrick M. McCarthy, M.D., of the Cleveland Clinic Heart Cen ter, performed the procedure for the first time at the Cleveland Clinic, one of the first hospitals in the country to offer ventricular remodeling. The procedure was developed in Brazil, where it has been performed on more than 300 patients.
The left ventricle is responsible for pumping oxygenated blood through the heart's aorta to the body. When the left ventricle does not function properly, the heart must work extra hard to provide this bl ood supply. Congestive heart failure causes the heart to increase in size to compensate for the left ventricle's inability to efficiently pump blood. Ventricular remodeling involves the resection (surgical removal) of a portion of the left ventricular muscle. This technique restores the ventricle to its optimal size and the efficient delivery of blood.
Not everyone is a candidate for ventricular r emodeling. The most appropriate treatment for your condition can only be determined by you and your physician. For some individuals awaiting a heart transplantation, ventricular remodeling may provide an alternative to the need for a heart transplantation. It is estimated that 30,000 Americans currently could benefit from a heart transplant, yet only 2,300 are performed each year due to donor shortages. The Cleveland Clinic Heart Center is pioneering the procedure as a another potential option for the treat ment of congestive heart failure.
Patients with symptomatic end-stage congestive heart failure may be appropriate candidates for ventricular remodeling. Each patient will be evaluated on a case-by-case basis by a Cleveland Clinic Heart Center physician. Patients on left-ventricular assistdevices for congestive heart failure may also be candidates.
Dr. Patrick McCarthy is a board-certified cardiovascular and thoracic surgeon. His area of special interest is heart failure, and he has the most experience with implantable left-ventricular assist devices in the world. He also performs heart transplant operations. In his medical career, Dr. McCarthy has performed thousands of cardiovascular surgeries. He completed a residency and fellowship in Cardiovascular Surgery at the Mayo Clinic and a Heart Transplantation and Assist Devices fellowship at Stanford University.
The Cleveland Clinic Heart Center is currently involved in the advancement of many new techniques aimed at treating patients with end-stage congestive heart failure and ultimately reducing the need for heart transplantation. These advancements include participation in clinical trials exploring the use of new drug therapies, permanent implantable left-ventricular assist devices, and cardiomyoplasty, a procedure that involves wrapping the back muscle (latissimus dorsi) around the heart and training it to behave as cardiac muscle.
Your hospital should have board-certified heart surgeons that have been trained in and have performed any surgical treatment. The Cleveland Clinic Heart Center has more experience with the Heart Mater left-ventricular assist device than any other cardiovascular program in the world. To date, the Heart Ce nter has implanted more than 90 assist devices, transplanted almost 500 donor hearts, and it continues to participate in cardiomyoplasty research.
If you think you may be a candidate, please call the Cleveland Clinic Heart Center at 800/822-9488. You will need to have your physician send your medical records including any prior cardiac catheterization.
The Cleveland Clinic Heart Center has pioneered the use of implantable left-ventricular assist devices and is one of the leading heart transplant centers in the country. Since ventricular remodeling is not an option for all end-stage congestive heart failure patients, these other treatment modalities will be available. Additionally, these other treatments (left ventricular assist devices and transplant) represent viable alternatives for medical conditions where ventricular remodeling is not effective.
The Cleveland Clinic Heart Center will work with your insurance carrier to ensure that you are not disqualified as a potential candidate for ventricular remodeling on the basis of availability of coverage.
For more information about Ventricular Remodeling please call the Cleveland Clinic Heart Center at 800/822-9488.
by Sulipsa Luque
LomaLinda, CA (7/10/96) Loma Linda University Medical Center surgeons carved a chunk of tissue from a Southland man's enlarged heart, giving him another chance at life with a radical procedure performed fewer than 20 times in this country.
Loma Linda doctors had run out of traditional ways to treat the enlarged heart of Roland Heights resident James Lyons, which no longer could pump an adequate supply of blood.
Physicians sent the 56-year-old man home last week to die with his family.
"We actually thought he would die within the next two to three days," said Dr. Thomas Heywood, Lyons' cardiologist and director of the Heart Failure Clinic at the Loma Linda International Heart Institute.
"We really had no options at that time, Haywood said. "It was such a severe condition, we couldn't even maintain his blood pressure."
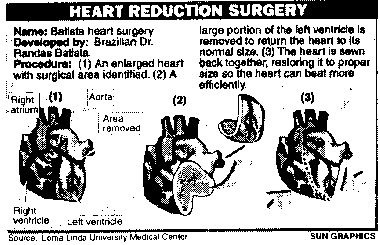
Then Haywood persuaded Dr. Steve R. Gundry, chief of the medical division center's division of cardiac surgery, to use the Batista heart surgery method, named for its developer, Brazilian surgeon Dr. Randas Batista.
The surgery requires removing a wedge of tissue from the heart, then sewing the organ back together.
"It's kind of crazy to think you can throw away one third of the heart and hope the patient does well," Gundry said. "While the heart was still beating, we opened up t he left ventricle and took out the muscle. Here he is two days later walking around the unit."
 Lyons had lived with a defective heart valve for 10 years before his condition worsened. His heart had grown to nine centimeters in diameter, nearly twice the normal five to six centimeters. The muscle was so stretched it was only a quarter-inch thick.
Lyons had lived with a defective heart valve for 10 years before his condition worsened. His heart had grown to nine centimeters in diameter, nearly twice the normal five to six centimeters. The muscle was so stretched it was only a quarter-inch thick.
Lyons kidneys started to fail because he had stopped taking heart medicine.
Sunday's three-hour surgery changed all that.
Now, his heat walls have relaxed so much that they are one inch thick and his kidneys are improving. Lyons is expected to go home next week.
He said he was undaunted by the experimental nature of the surgery.
"It came down to the point where I didn't have much of a choice on what I could do," said Lyons, a structural iron worker until illness forced him to quit.
"Today, I feel great - a little sore - but in a couple of days I' I1 be ready to go. The thing is that you don't know how long it is going to last, but it is better than what I had."
Batista has performed the surgery about 300 times in two years, but it was not until a recent feature on ABC's news magazine "20/20" that people began asking about the procedure, Gundry said.
"We were jumping up and down," said Tracy Hernandez, Lyon's daughter, of the doctors' decision to do the surgery. "We were happy. The whole family was bursting because we had hope instead of nothing."
The more d octors perform the surgery the more they will learn about the amount of muscle to cut out and who makes the best candidates are for the procedure, Gundry said.
About 40,000 people die of heart failure each year in the U.S. The surgery could help reduce that number, Gundry said.
"It's a dangerous operation, there is no doubt it," Gundry said. It goes against all our surgical training, but it beats the alternative to go home and die."
Heywood said the Batista surgery also migh t save thousands of people on heart transplant waiting lists by buying them time or eliminating the need for a new heart.
"We are trying to stretch what we can do with ordinary surgery, so we can save transplants for those who really need it," Heywood said. As for Lyons, he is looking forward to getting back to as normal a life as he can have. "Right now I feel like playing football."
The San Bernardino Sun, July 10, 1996
Contributed by Tx Stewart Lilley, Victorville, CA (As of August 8th, Mr. Lyon has often been unavailable .... because he's out fishing/Ed.)
If you're really proud of your transplant, maybe you should consider purchasing a likeness cast in sterling silver. Now available from Sacredbody are pins representing the heart, lungs and trachea, kidney with adrenal, liver and gall bladder, and what the hey, even the internal reproductive organs for those really feel a need to wear their organs on their sleeve so to speak. They all retail for $30 each plus shipping from Sacredbody, P.O. Box 91, Vermillion, SD 57069, 1-800-203-8299.
For those who surf the Intemet for the cultural materials, there's a new Website with a free search ability of Medline the large medical data base. It can b e found at http://www.healthgate.com/HealthGate/ MEDLINE/search.shtml. So far this site seems to benot one of those that captures your name for Spam purposes. Also keep in mind that such data bases can make for quite stultifying reading as they are not meant for educating the general public.
BONN, Germany (Reuter 6/12/96) - Surgeons in southern Germany said they had performed the world's first knee transplant operation on a 17-year-old youth, who smashed his leg in a motorcycle accident, German television reported Wednesday.
Doctors in the Bavarian town of Murnau said they had successfully replaced the youth' s knee with a donor knee in April in an operation that lasted 14 hours, ARD television said.
It said that the knee can now bend and has a blood supply. (Which is more than can be said for the guy's brains. Ed.)
BONN,(Reuter 7/26/96) - A German surgeon not only performed a successful kidney transplant operation, but also provided the donor organ himself, a German radio station reported on Friday.
"The idea resulted from a talk with colleagues who said we should only recommend to our patients what we would do to ourselves,&qu ot; Dr. Jochen Heuer, 53, told German NDR radio.
Heuer, who is a medical professor from the north German port of Luebeck, said both he and his patient had felt fine since the operation, but they had not developed a friendship. "I wanted to stay anonymous and out of the headlines," he added. (And hereto is yet another indication that IQ is not really an indication of smart. Ed.)
I've was once told by a fellow Tx that he figured just about the dirtiest thing he ever comes in contact with is the handle on the supermarket shopping cart. When you consider, he's probably very right, especially when you think of the runny nosed kid whowas riding the "shotgun pocket" a few minutes before you picked it up. Ever since l've kept a box of Wash N Dri's in the center console of the car for just such emergency handwashing.
By Sam Greene
Bardstown, Ky. Three brothers who shared so much in health now share even more in sickness. All stricken with a rare and terminal heart disease, they wait together for scarce heart transplants.
How long they will live is uncertain, but their lives as they knew them are over.
Doug Greenwell, at 32, is both the youngest and the sickest of the three, all o f whom have been diagnosed with dilated cardiomyopathy, which causes the walls of the heart to balloon so that the organ does not pump efficiently.
Keith, 35, and Ron, 36, have similarly enlarged and weakened hearts in different stages of the incurable disease, inherited in this case.
Shortly after Doug was diagnosed, the brothers dug up records showing that their father, who died at 45, also suffered from cardiomyopathy. Their mother died of unrelated illnesses last year, and their two other br others have not been diagnosed with the disease. It is a rare disease, generally afflicting fewer than 35,000 people nationwide. That is would happen to three out of five brothers, said their doctor, is rarer still.
Because any physical or emotional stress could kill them, the brothers had to quit jobs they loved. The inactivity is hard to deal with, but necessary.
"It's something you have to get used to," Ron said. "You have to."
Untreated, the brothers could live for five or six more years, according to Raible, a cardiologist at Jewish Hospital in Louisville, Ky. Or they could die tomorrow.
"The nights you go to bed when you don't feel so good, you think, 'If I go to sleep, am I going to wake up in the morning?'" Keith said. "But you have to go to sleep."
The only long-term hope for the brothers is heart transplants.
Doug's condition is already so advanced that he has been put on the official transplant list; his brothers will event ually go on the list, their doctor said. After a name goes on the list, the average wait is 180 days. But because there is a shortage of donors and because a heart must be a perfect match, the wait can be years. Given the disease' s unpredictability, that' s a daunting fact.
When the brothers were diagnosed with cardiomyopathy last year, one of the first things they had to do was quit their jobs. The disease severely weakens the heart the heart, and physical or psychological stress can be deadly.
< P>It's a change from the lifestyle they've had since they were boys growing up on a farm in Kentucky's Marion County. They were always out in the fields, they said, either working the ground, mending fences or tending to the crops."You couldn't slow us down," said Ron. "That's what's difficult - slowing yourself down. We know we have to, and it's hard. It's getting a little easier, but not quite."
As adults, the brothers share a passion for trucks. Ron worked as a truck driv er before becoming manager of the Fast Lube in Bardstown. A year and a half before diagnosis, Doug and Keith realized a lifelong dream by opening a truck repair shop, working onheavy rigs.
All three used to start their days about 6 in the morning, working until 8 p.m. or sometimes 10 or 11.
"It's something we enjoyed doing," Keith said. "It's hard, dirty work, but it takes a certain kind of person to be a good mechanic."
All three stay home now, seeing their kids off to school and their wives off to work in the morning. About 10 or 11 a.m., one of them usually calls another to plan the day.
Just to get out of the house, they accompany each other on errands. Sometimes they go to Doug and Keith' s old shop to talk with the new owners. Every once in a while, they'll go out for a bite to eat.
Children and family have become more important for them now, although there are frustrations.
"I didn't have time to do much before I got sick," Keith said wh en talking about his 14-year-old daughter. "Now there's not that much I can do."
Ron put up a basketball hoop out back for his 9-,15-and 18-year-old boys last summer. Now he can't even shoot baskets with them.
Doug stays at home in the afternoons with his 4-year-old son, riding him around the lawn on the mower or pushing him on the swing.
When the weather's warm, Doug said he and his wife, Stephanie, like to go to the park with their son and just sit and watch him play.
Mar ty Justice of Bardstown, a friend whose 3-year-old son plays occasionally with Doug's son, said Doug, like his brothers, has dealt with his disease well, planning for the inevitable while never letting the tragedy of it keep him from enjoying life.
"I've been encouraged by his attitude," Justice said. "I would hope I'd have the same attitude under those conditions."
Last year all three brothers began to notice their rigorous routines were making them more tired than usual.
"It was run, run, run all day," Ron said. "We were nonstop, 24 hours a day. I kind of felt funny. It felt different, but I kept on pushing."
But in July, Doug couldn't push anymore. He went to the doctor, where they drained fluid from his lungs. Soon afterward he was diagnosed. The same happened in December for Ron and Keith.
The need for transplants - and what one means for their future - hangs over the brothers' heads, just as it hangs on Doug's belt.
"When I get one of those beepers," Ron said, "when that thing goes off, everything from your lifetime is going to flash through your head in that 45 minutes to drive to the hospital."
Raible stresses, however, and has stressed to the brothers, that a transplant is not a cure. It's a treatment, with very serious side effects. Even in the best case, the brothers will have to take antirejection drugs for the rest of their lives, leaving them open to infection. Just like the disease, the outcome i s unpredictable.
"Many people return to full activity," Raible said. "Some even go back to work. It's all really individual."
Doug knows, probably better than his brothers, that he is moving closer to something, either a transplant or death.
And so he, more than his brothers, has given a lot of thought to what that moment, after the beeper sounds, will be like.
"I'm going to be lying on that table and they're going to take my heart out and put in a new one, a nd I'm not even going to know it," he said. "You know you could die on that operating table. I'm going to die either way. To get the transplant, though, andlive through it, that's something to look forward to."
Washington Post-Health 5/14/96 Submitted by Myrna Porter, Woodbridge, VA
By Kevin Draw baugh
CHICAGO (Reuter 7/17/96) - Heart surgeons on the cutting edge are trying to minimize the cutting.
Techniques are being tested at several U.S. hospitals for operating on the heart without the usual first steps -- making a long incision in the chest, sawing the breastbone in half and prying open the rib cage.
The new "minimally invasive" techniques eliminate these steps by enabling the surgeon to cut small access ports in the chest and operate on the heart using long, probe-l ike instruments. Some surgeons are combining them with new equipment that allows them to work on a heart that is still beating, eliminating another standard step in open-heart surgery -- putting the patient on a heart-lung bypass machine.
Taken together, these breakthroughs are altering the way physicians approach the most common type of major operation performed today in the United States. "This is a revolution in heart surgery. It's going to change the whole thing," said Dr. Valavanur Subr amanian of Lenox Hill Hospital in New York.
Surgeons like Subramanian are touring the world now making presentations to their peers about the new techniques. A conference was held late last month in Minneapolis and another is scheduled for this month in Montreal.
"I've been asked to give over 20 talks in the past six months on this. Everytime I go into a conference room there are people hanging out the doors," Dr. Tom Burdon of Stanford University in California said. In a few years, Bu rdon said, minimally invasiveheart surgery will be commonplace. "It's just a matter of the number of people that feel comfortable doing it and getting them trained, and that's happening now."
Heart disease is the leading U.S. cause of death. Each year, 1.5 million people undergo heart surgery of some sort at a cost per procedure ranging from $15,000 to $55,000.
For many, that means open heart surgery, where the chest is cracked and a diseased heart artery or valve is replaced. For othe rs, it means angioplasty, where an instrument is inserted through a catheter into a clogged heart artery to clean it out and, if needed, shore it up.
These procedures have saved millions of lives, studies show, but not without risks and costs. Recuperation from open heart surgery takes eight to 10 weeks, without post-operative infection, and leaves the patient with a large and permanent scar down the chest. The patient's circulatory system and brain are also stressed if, as is typical, the heart is st opped and the patient is hooked up to a heart-lung bypass machine that pumps and oxygenates the blood during surgery.
Angioplasty can be done without a major incision or a bypass machine but recent studies are questioning the long-term effectiveness of these procedures. With these problems and limitations in view, more surgeons are trying the new minimally invasive techniques.
Dr. Mario Pompili of Stanford and the Palo Alto, California Veterans Administration Hospital, who has done 12 heart oper ations using equipment developed by Heartport Inc, said "The most rewarding aspect of it is we're able to perform the operation throughvery small incisions."
Heartport's Port-Access CABG system allows coronary artery bypass grafts to be done through four small chest access ports. Its PortAccess MVR system permits heart valve replacements to be done through ports.
Both procedures still require a stopped heart and a bypass machine but eliminate the need for cracking the chest.
The company expects its equipment to be used in 75 to 200 operations this year by specialists working in more than 20 hospitals. So far, Heartport gear is used only in clinical trials and has not been approved by the U.S. Food and Drug Administration for full-scale commercialization.
Site Stats: