

By Jeffrey D. Hosenpud, MD et al
[Editor's Note: In the interest of comprehension (see PVC's) UpBeat will only include a brief summary of the major facts and statistics from this now 22 page report, and then include a few of the graphs.]
The Registry now contains data on 45,993 heart transplantations reported from 301 heart transplantation programs. The cut off date for the last 12 months of data was March 1, 1998.
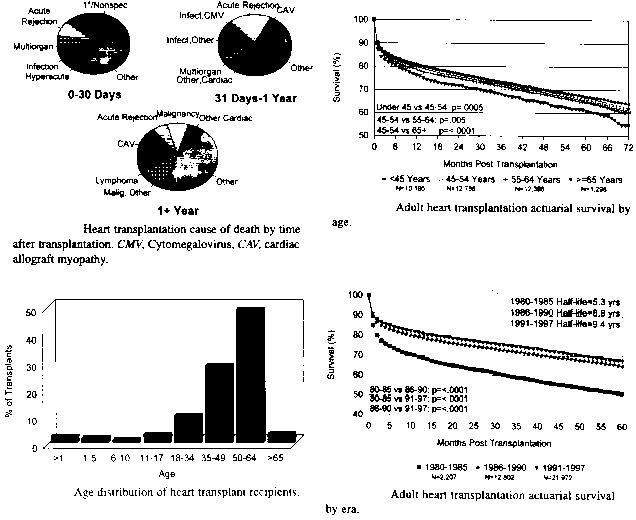
Using data collected over the past 13 years, the 1 year actuarial survival after heart transplantation is 79*/0. After 10 years the survival rate is 42%. For a patient surviving the first year the 1/2 life (time to 50% transplant population survival) is 11.4 years. However, the year of transplantation also has a major bearing on survival statistics.
Year of Tx Tot. Number Half-life
1980-1985 2,207 5.3 yrs.
1986-1990 12,802 8.8 yrs.
1991-1997 21,972 9.4 yrs.
There is a statistically significant decrease in survival for each increase in decade of life, with a clinically significant decrease in those patients over age 65 years.
 Again
interesting and probably worthy of further sociological research is
the fact that while most patients are considered to have no
limitations in function, less than 40% are working (and does not
include those retired).
Again
interesting and probably worthy of further sociological research is
the fact that while most patients are considered to have no
limitations in function, less than 40% are working (and does not
include those retired).
Maintenance immunosuppression shows that while the great majority of patients are using cyclosporine and azathioprine, a growing number of patients are being treated with tacrolimus or mycophenolate mofefil. However, more than 75% are still on corticosteroids at 3 years after transplantation.
In the first 30 days after transplantation, nonspecific graft failure accounts for the largest proportion of deaths. From 30 days to one year, there is approximately equal death rate due to either acute rejection or infection. From one year out, using the entire data set, the most common causes of death are cardiac allograft vasculopathy, malignancy, and, interestingly, acute rejection.
PVCS
When UpBeat first started, the entire Registry Annual Report was contained in about 4 or 5 pages of the Journal of Heart & Lung Transplantation. UpBeat readers were able not only to understand the report, but nearly the entire data could be included in one newsletter article. I hate to say it, but shortly after UNOS entered the program about a year and a half ago the report seems to have become a product of bureaucracy at its highest level of practice.
The report now consumes 12 pages. Granted it has excellent graphics, although precise interpretation of same is somewhat difficult due to small size. But it also has left the layman (read transplant recipient) in the litter of its scientific lingo. For just a single example, the following is one sentence of many like it from the opening page of the report:
"A multivariate logistic regression analysis was then applied to the entire data set, but limited to those patients who had all of the model variables available in their records to determine the independent predictors of survival."
Wow, talk about the origin of "Richmond we have a problem."
![]()
Still, yet, again many thanks for the kind words that appeared after the renewal of UpBeat late last month. Both well wishes and donations have come in at a surprising rate. As usual there will be no December issue, which used to be good for a break, but this year will be fairly well consumed with some more "throat spelunking."
The happiest of Holiday Seasons to one and all. Stay well, but as the late heart recipient Dr. Mike Eisenman of Tucson used to say, "Remember one or two meals of things that taste great, but are bad for you, should be totally enjoyed. They sure won't kill you."
By The Associated Press - 9/7/1998
A list of organ procurement organizations and the number of transplants enabled per 1,000 deaths. The figure is an average of two years, 1996 and 1997. The list also includes the location of each group's headquarters and a description of its territory.
Institutions with higher numbers enabled more transplants, potentially saving more lives:
University of Wisconsin, 146.01 Madison, Wis.; Wisconsin except area surrounding Milwaukee
LifeSource, 99.94 St. Paul., Minn.; Minnesota, North Dakota, South Dakota, two counties in Wisconsin
Intermountain Organ Recovery Systems, 97.60 Salt Lake City; Utah, southern Idaho, southwest Wyoming
Southern California Organ Procurement Center, 95.15 Los Angeles; part of the Los Angeles area
Wisconsin Donor Network, 93.43 Milwaukee; 11 counties in eastern Wisconsin
Organ and Tissue Center of Southern California, 85.26 San Diego; Imperial and San Diego counties
Washington Regional Transplant Consortium, 82.59 Washington, D.C.; Washington plus Maryland and Virginia suburbs
Lifeline of Ohio, 78.79 Columbus, Ohio; Columbus, Mansfield, southeast Ohio, part o West Virginia
LifeLink of Florida, 75.48 Tampa, Fla.; Tampa area
Donor Alliance, 74.74 Denver, Colorado, most of Wyoming
TransLife, 71.88 Orlando, Fla.; Orlando area
NorthEast OPO, 71.23 Hartford, Conn.; most of Connecticut, western Massachusetts
Pacific Northwest Transplant Bank, 70.76 Portland, Ore.; Oregon, parts of Washington and Idaho
Golden State Donor Services, 65.84 Sacramento, Calif.; nine California counties
Iowa Statewide OPO, 65.66 Iowa City, Iowa; most of Iowa, one Nebraska county
LifeLink of Georgia, 64.90 Atlanta; most of Georgia, two counties in South Carolina
Delaware Valley Transplant Program, 63.57 Philadelphia; Delaware, eastern Pennsylvania and part of New Jersey
Kentucky Organ Donor Affiliates, 62.13 Louisville, Ky.; most of Kentucky, small parts of Indiana, Ohio and West Virginia
Nebraska Organ Retrieval System, 61.94 Omaha, Neb.; most of Nebraska, one Iowa county
California Transplant Donor Network, 60.25 San Francisco; 40 counties in California
Center for Organ Recovery and Education, 59.60 Pittsburgh; western Pennsylvania, part of West Virginia
Southwest Transplant Alliance, 57.02 Dallas; 90 Texas counties mostly in northeast
Mid-America Transplant Services, 55.82 St. Louis; eastern Missouri, southern Illinois, small part of Arkansas
University of Florida, 55.58 Gainesville, Fla.; northern Florida
Tennessee Donor Services, 54.28 Nashville; most of Tennessee, small parts of Georgia and Kentucky
Life Gift Organ Donation Center, 51.72 Houston; 108 Texas counties mostly in northwest
Midwest Organ Bank, 51.27 Westwood, Kan.; Kansas, western Missouri
Fingerlakes Donor Recovery Network, 50.27 Rochester, N.Y.; 19 New York counties
Ohio Valley LifeCenter, 50.09 Cincinnati; southwest Ohio, small parts of Indiana and Kentucky
LifeShare of the Carolinas, 49.89 Charlotte, N.C.; part of North Carolina, one county in South Carolina
LifeNet, 49.88 Virginia Beach, Va.; eastern Virginia
Donor Network of Arizona, 49.58 Phoenix; most of Arizona
Regional Organ Bank of Illinois, 49.25 Chicago; most of Illinois, small parts of Indiana and Iowa
Indiana Organ Procurement Organization, 48.76 Indianapolis; most of Indiana, one county in Kentucky
Life Connection of Ohio, 48.33 Maumee, Ohio; western Ohio
South Texas Organ Bank, 47.93 San Antonio, Texas; 56 Texas counties in central, southern and eastern Texas
Life Resources, 47.08 Johnson City, Tenn.; southwest Virginia and northeast Tennessee
Center for Donation and Transplant, 46.97 Albany, N.Y.; 23 New York counties, one Vermont county
Alabama Organ Center, 46.86 Birmingham, Ala.; Alabama and three Georgia counties
Arkansas Regional Organ Recovery Agency, 46.29 Little Rock, Ark.; most of Arkansas
University of Miami Organ Procurement Agency, 45.32 Miami; southern Florida
LifeBanc, 43.69 Cleveland; northeast Ohio
Mid-South Transplant Foundation, 43.39 Memphis, Tenn.; parts of Tennessee, Arkansas and Mississippi
LifeLink of Southwest Florida, 43.25 Tampa, Fla.; Fort Myers area
New England Organ Bank, 42.08 Newton, Mass.; Rhode Island, Maine, New Hampshire, most of Vermont, most of Massachusetts, New Haven area of Connecticut
Transplant Resource Center of Maryland, 41.83 Baltimore; Maryland except D.C. suburbs, one West Virginia country
Carolina Organ Procurement Agency, 41.61 Greenville, N.C.; eastern North Carolina, two counties in Virginia
Transplantation Society of Michigan, 41.55 Ann Arbor, Mich.; Michigan
Louisiana Organ Procurement Agency, 41.09 Metarie, La.; Louisiana
New Mexico Donor Program, 38.90 Albuquerque, N.M.; New Mexico
New Jersey Organ & Tissue Sharing Network, 38.59 Springfield, N.J.; most of New Jersey
Virginia's Organ Procurement Agency, 37.94 Midlothian, Va.; western Virginia
Nevada Donor Network, 37.80 Las Vegas, Nev.; Nevada, one Arizona county
Carolina LifeCare, 35.29 Winston-Salem, N.C.; western North Carolina
Organ Donor Center of Hawaii, 34.30 Honolulu; Hawaii
South Carolina Organ Procurement Agency, 34.27 Charleston, S.C.; most of South Carolina
Upstate New York Transplant Services, 33.10 Buffalo, N.Y.; seven New York counties
New York Organ Donor Network, 25.40 New York City; New York City area, Long Island
Regional Organ Procurement Agency of Southern California, 25.26 Los Angeles; part of the Los Angeles area
Mississippi Organ Recovery Agency, 17.80 Jackson, Miss.; most of Mississippi
LifeLink of Puerto Rico, 29.5 Guaynabo, P.R.; Puerto Rico and American Virgin islands ..
Note:
Two organ procurement agencies are not included in this ranking because data was unavailable on the number of deaths in the area, making a calculation of transplants per death impossible. The Oklahoma Organ Sharing Network in Oklahoma City is not included because the state does not report death data to the Centers for Disease Control and Prevention. LifeCenter Northwest, which covers Alaska, Montana and most of Washington, is not included because it is a product of two organ banks that recently merged. There is no reliable death data for the new entity. It is, however, possible to calculate the number of transplants performed for every 1 million people living in these areas. This is the standard that the government uses to judge organ banks.
Using the population standard, the Oklahoma Organ Sharing Network, which covers the state of Oklahoma, ranked No. 52 out of 63 organ banks. It performed an average of 54.46 transplants per year in 1996 and 1997 for every 1 million people. LifeCenter ranked No. 56, performing 52.65 transplants for every 1 million people.
Southern California Jewish Community Unites To Promote Program That Saves Lives; Houses of Worship To Raise Congregants' Awareness November 13-15
Woodland Hills, Calif.--(BW HealthWire)- 10/ 26/1998--While 56,000 people in the United States remain on the national waiting list for an organ donation and an average of ten individuals die each day while waiting, a Southern California organization has taken a "don't wait, motivate" approach to increasing organ and tissue donations.
Transplant For Life, a group affiliated with the Irving Grant Service Center at Temple Kol Tikvah (Voice of Hope) in Woodland Hills, California, has created a grassroots program to promote and encourage participation in the countrywide National Donor Sabbath, launching its effort with the entire Jewish community of Southern California. The group's slogan is "miracles through understanding."
Scheduled for Nov. 13-15 this year, National Donor Sabbath was developed by the U.S. Department of Health Resources and Services Administration in 1996 as a way to make clergy and their congregations aware of the critical need for organ and tissue donation. The second weekend in November was selected for its proximity to Thanksgiving, viewed as an appropriate interfaith time to come together around the issue of valuing and giving life. Based on a recent Southern California survey, however, less than 10 percent of all houses of worship have participated in this annual event. Thanks to the proactive efforts of Transplant For Life, the results this year should be dramatically different.
"Our primary objective is to act as a catalyst for increased donation by helping synagogues and temples in all branches of Judaism in Southern California become active and united participants in this national effort," said Irv Goldberg, chairman, Transplant For Life. "We believe our rabbis as teachers can be highly effective in bringing this issue to their congregations. During National Donor Sabbath, our clergy will address the importance of organ and tissue donation.
 "Our
action doesn't end with National Donor Sabbath," Goldberg
continued. "Transplant For Life will work to extend this
increased awareness and participation into a year-round program, to
support model programs and related legislation, and to encourage
other religious organizations of all affiliations to enact similar
programs, using our pilot program as a model."Transplant For
Life's project has received the unanimous endorsement of the Southern
California Board of Rabbis, representing all four branches of Judaism
(Orthodox, Conservative, Reform and Reconstructionist). This united
support underscores the little known fact that, according to Jewish
tradition, organ donation is not only permitted but actually
commanded. In his Yom Kippur sermon this year, Rabbi Steven Jacobs of
Kol Tikvah addressed the subject as follows:
"Our
action doesn't end with National Donor Sabbath," Goldberg
continued. "Transplant For Life will work to extend this
increased awareness and participation into a year-round program, to
support model programs and related legislation, and to encourage
other religious organizations of all affiliations to enact similar
programs, using our pilot program as a model."Transplant For
Life's project has received the unanimous endorsement of the Southern
California Board of Rabbis, representing all four branches of Judaism
(Orthodox, Conservative, Reform and Reconstructionist). This united
support underscores the little known fact that, according to Jewish
tradition, organ donation is not only permitted but actually
commanded. In his Yom Kippur sermon this year, Rabbi Steven Jacobs of
Kol Tikvah addressed the subject as follows:
"The promise of saving people's lives through organ transplantation is for Judaism and most other traditions of supreme importance. Organ transplantation has become possible only in the second half of the 20th century. It should not be surprising then that classical Jewish sources, written hundreds, if not thousands, of years ago have nothing specifically to say about transplantation. Yet for a living tradition like Judaism, it only means that concepts, values, practices and laws from the past must be applied to this new technological possibility just as they are to many other new realities.
"We are bidden in the book of Leviticus to obey God's commandments v'chai vachem and live by them. The rabbis of the Talmud deduced that this means we should not die as a result of observing them. The tenet that emerges is one of the great Jewish insights of all time, pikkuach nefesh, the obligation to save people's lives... Judaism' s over-arching command is to save life and limb and has prompted all rabbis who have written on the subject to indeed urge us as Jews, and non-Jews, to make provision for donating our parts..."
Transplant for Life has set a goal in 1998 of achieving a 100% increase over 1997 in participation of the National Donor Sabbath. To realize this goal, the organization has broadcast a priority fax to approximately 100 rabbis in the Southern California area, seeking their participation. Each clergy is given a form to be completed, ascertaining the steps they will take to. address the national event. These actions may include giving a sermon, inserting a brochure into the congregation' s bulletin, inviting a speaker, referring to organ/tissue donation in the bulletin, distributing donor cards/brochures, and using relevant scripture.
In addition to addressing their own congregations, participating rabbis are asked to encourage other Jewish clergy to include the topic in their Sabbath services on Friday evening, November 13, and Saturday, November 14. Transplant For Life is prepared to help rabbis by providing materials, sample sermons and bulletins, scriptural references and educational materials.
"Family communication is crucial for solving the shortage of donor tissue and organs," added Goldberg. When a death occurs, hospitals request consent for donation from the next-of-kin. Thus, it is critical that family members know each other's wishes about donation before a death occurs. "Rabbis addressing the issue of donation are often the catalysts for those discussions," said Goldberg.
National Donor Sabbath is endorsed by the Coalition on Donation, including the American Diabetes Association, American Heart Association and the American Kidney Foundation, among other organizations. Materials about organ and tissue donation may be ordered from the:
Union of American Hebrew Congregations, the United Synagogues of Conservative Judaism, the Union of Orthodox Jewish Congregations, the Division of Transplantation, and the United Network for Organ Sharing.
Transplant For Life is prepared to help expedite the materials requested. Transplant For Life may be contacted at:

London, Nov 4, 1998 (Reuters) - Japanese scientists have developed a method of storing organs which could transform the transplant industry, a science magazine said on Wednesday.
Borrowing a trick from a tiny bug called a tardigrade that can survive under extreme conditions, scientists at Kanagawa University in Japan have revived a rat's heart after 10 days in storage, 10 times longer than normal.
"The team... says the work may lead to organ banks similar to blood banks," New Scientist magazine said.
A lack of available human organs is a daunting problem for transplant surgeons. Organs often become available at the last minute and there is a frantic rush to get them to patients in time to save them.
If scientists could store donated organs for long periods of time, it could open up new opportunities for patients and lead to better matches between donors and recipients.
Using current techniques, the longest human organs can be stored is up to about 30 hours. For livers and hearts the storage time is only about four hours.
But the Japanese technique, developed by Kunihiro Seki and his colleagues, could change that, thanks to the tardigrade which uses a sugar called trehalose to survive in extreme conditions.
"The main problem with keeping organs in cold storage is that water damages cell membranes at low temperatures. Unfortunately, removing water from tissues usually causes at least as much damage," the magazine said.
To overcome the problem the researchers flushed rat hearts with trehalose solution and then packed them in silica gel to remove the water from the cells. Then they immersed the hearts in a biologically inert compound called perfluocarbon and stored them in airtight jars at 4 degrees Centigrade (39.20F).
Ten days later they removed the hearts and revived them.
There appeared to be no damage to the heart cells.
"Seki believes that the trehalose and perfluorocarbon replace the water in cells, preventing tissues damage," the magazine added.
The Japanese researchers plan to test the technique on other animal organs. If all goes well, they hope the method could be used for preserving human organs in a few years.
Novartis does not view SangStat's new drug as a threat to its market share, which accounted for $1.35 billion in revenues worldwide in 1997, said Jeff Cook, a company spokesman.
"We believe that the medical transplant community will view the entrance of any new cyclosporine with caution," he said.
Additionally, S angStat's drug is a drink solution, which Cook said is used for a very small portion :of transplant patients.
"Less than 5% of Neoral patients are on the drink solution," Cook said. Novartis' Neoral cyclosporine is marketed in capsule and drink solution form, Cook said.
John Davis, the executive director of the National Kidney Foundation, said he can't predict how the pharmaceutical sector or the medical community will react to SangCya's launch. The group is concerned, however, that kidney transplant patients be notified of any switch in their cyclosporine medications by their doctors or pharmacists, Davis said.
"We don't think a patient should be given something else without being taught about the differences between the drugs and the effect it has on their bodies," Davis said.
If a patient were to receive too small a dose of the immunosuppressive or cyclosporine drug he or she could reject the transplant. Lund said SangCya' s acceptance in the medical community is a concern of Mehta Partners.
"Because this is a very delicate market and all cyclosporine patients are being treated with Novartis' drugs, doctors may be worried about switching patients over to SangCya," Lund said.
While Lund said the drugs are equivalent, he expects patients will be transferred gradually to the cheaper SangCya treatment.
"Within two months, or so, we will see some prescription data," Lund said.
"So a lot depends on Novartis and the prescriptions. We are telling our customers this is basically a hold situation until we see some other improvements."
Dow Jones, 11/3/1998
By Patricia Zengerle
Miami (Reuters 10/30/1998) - A Florida man became the first person in the United States to receive a transplanted organ from a donor in South America this month when surgeons gave him a new liver from a Bolivian, doctors said Friday.
Richard Del Gais, 55, of PlantatiOn, Florida, received his new liver on Oct. 13 during a 13-hour operation at the University of Miami' s Jackson Memorial Hospital. He was discharged from the hospital in good condition on Friday.
Diagnosed with Hepatitis C, Del Gais had spent a year on the hospital' s waiting list for a donor liver without a compatible organ becoming available.
The organ from Bolivia became available in Miami after Dr. Steven Dunn, a transplant surgeon from St. Christopher's Hospital for Children in Philadelphia, went to Bolivia to assist with a liver transplant from a living donor.
While there, authorities told him that a donor liver had become available, but was not going to be used in the South American nation.
The donor's kidneys were to be used locally, but there was no liver recipient available, so local authorities asked Dunn if it could be used in the United States.
"They had a local donor and they told him... they didn't have a match for the liver," Dr. Andreas Tzakis, director of the University of Miami/Jackson Hospital Liver/Gastro Intestinal Transplant Program, told Reuters.
Dunn contacted the United Network for Organ Sharing, the agency that coordinates organ distribution in the United States, and it arranged the match with Del Gais.
UNOS has arranged transplants in the United States from about 300 foreign donors, virtually all of them in Canada, since 1988. But it said this was the first instance of a transplant in the United States from a donor in South America.
There is a chronic shortage of donor organs in the United States. Although 15,000-20,000 deaths per year could result in a donated organ, relatively few are donated.
U.S. officials say 4,000 Americans die every year while waiting for organ transplants.
Tokyo (AP 10/28/1998) -- Doctors at Okayama University Hospital in western Japan carried out the country's first lung transplant from living donors today. Organ transplants have been extremely rare in Japan because of a previous law that recognized death only after a patient's heart stopped beating. At that point, organs such as hearts and lungs are usually unsuitable for transplant.
A year ago, a new law was passed to recognize brain death.
Still, the idea of removing organs still meets tremendous resistance because of a widespread distrust toward doctors as well as cultural superstition about cutting into corpses. Not a single transplant has been performed in Japan from brain-dead donors.
Today, a 24-year-old woman with an incurable lung disease received half of her 48-year-old mother's left lung and one-third of her 21-year-old sister's right lung.
All three, whom the hospital did not identify, were in stable condition after the nine-hour surgery, a hospital official said. Dr. Nobuyoshi Shimizu led a team of 20 doctors in performing the operation. The recipient was expected to recover to about 50 percent of her lung capacity, the newspaper Yomiuri said today. In the last month before surgery, an artificial respirator was helping her breathe.
The donors' lung functions will be reduced by about 20 percent, but they will be able to lead regular lives, the paper said.
A 1996 medical study found that about 400 Japanese patients needed lung transplants during a two-year period, and as many as 3,000 patients now awaiting lung transplants, the Yomiuri said. Some patients flew abroad for transplant operations.
Doctors here have performed lung transplants before but never using organs from a living donor. The most common organ transplants from dead donors carried out in Japan are kidney and cornea transplants.
By Ravi Nessman - Associated Press Writer NEW YORK (AP) -- Ketil Moe is not sure he'll make it to the finish line of the New York City Marathon. Simply making it to the starting line will be a huge accomplishment. He is, after all, running with a new set of lungs.
Moe is one of six transplant recipients who plan to run the marathon on Sunday, and he most likely is the first lung recipient to tackle a course this long, according to Dick Traum, president of the Achilles Track Club for disabled athletes.
Moe, a 31-year-old diabetic, had to suck oxygen and use a wheelchair before his double lung transplant in the summer of 1997.
"If I can get through the race, I know that I have my disease under control," he said.
Speaking from his home in Kresteansand, Norway, Moe worried that a lingering bacterial infection might prevent him from running.
His doctors warned him not to do it. But they also warned him about many of the 12 marathons he had ran before his transplant, races he sometimes entered with bleeding lungs. This time he plans to run slowly, with his doctor, his physical therapist and two Norwegian champions, former marathoner Grete Waltz and Johann Olay Koss, an Olympic gold medalist speedskater.
"I hope I will survive," he said with a slightly wheezing laugh. "It will be the toughest race ever."
Running a marathon is not a good idea for most transplant patients, said Dr. Niloo Edwards, surgical director of heart transplants at Columbia Presbyterian Hospital in New York. But those healthy enough to do it are a symbol of hope for sick people leery of the surgery.
"It' s a testament to how well transplantation works in the 1990s and to really how much quality of life... the gift of these organs brings to these patients," Dr. Edwards said.
For Donald Arthur, the transplant itself led him to the marathon. He began race walking to counter the bone atrophy resulting from his antirejection drugs.
Traum quickly persuaded him to enter last year's marathon, an event he never cared about before his heart transplant two years ago.
"The only thing I used to do with a marathon was sit in my chair with a beer and a cigarette and the remote control and change the channel because I didn't want to see anyone in that pain and agony," the 54-year-old New Yorker said.
Smoking and drinking, combined with a cocaine habit, made Arthur's already diseased heart grow monstrously large and nearly shut it down.
"I couldn't talk anymore because I was gasping for air," he said. "It took over half an hour for me to walk a city block."
He respects his body now. To do any less would dishonor the 25-year-old man he knows only as Fitzgerald. The man whose heart keeps him alive.
Arthur inspired Maria Jimenez to run after she received a transplant of her mother's kidney.
The 35-year-old freelance illustrator spent three years suffering through exhaustive dialysis treatments after lupus destroyed her kidneys. Now she wants to make sure she takes full advantage of her mother' s gift.
"I just kind of want to feel life again after feeling so limited for so long," she said.
 Arthur's
voice quivers and he begins to cry as he talks of the new life
Fitzgerald' s family gave him when they cleared their minds of grief
long enough to donate the man' s heart.
Arthur's
voice quivers and he begins to cry as he talks of the new life
Fitzgerald' s family gave him when they cleared their minds of grief
long enough to donate the man' s heart.
Arthur is dedicating his race this year to them and to all the families who have made the same painful,dec,ion, and to the patients who died waiting for transplants.
"It's all for them," he said. "It's their 26.2 miles."
Site Stats: